Artificial Intelligence For Healthcare Payer Market Report 2026

Artificial Intelligence For Healthcare Payer Market Report 2026
Global Outlook – By Component (Software, Services), By Technology (Machine Learning (ML), Natural Language Processing (NLP), Other Technologies), By Deployment (Cloud, On-Premises), By Application (Claims Processing Optimization, Fraud Detection and Prevention, Revenue Management and Billing, Member Engagement and Personalization, Risk Adjustment And Predictive Analytics, Administrative Workflow Automation, Other Applications) - Market Size, Trends, And Global Forecast 2026-2035
Artificial Intelligence For Healthcare Payer Market Overview
• Artificial Intelligence For Healthcare Payer market size has reached to $2.89 billion in 2025 • Expected to grow to $6.81 billion in 2030 at a compound annual growth rate (CAGR) of 18.6% • Growth Driver: Growing Volume Of Healthcare Data Fueling The Growth Of The Market Due To Increasing Digitalization And Data Availability • Market Trend: AI-Powered Platform Improves Efficiency And Reduces Burden • North America was the largest region in 2025 and Asia-Pacific is the fastest growing region.What Is Covered Under Artificial Intelligence For Healthcare Payer Market?
Artificial intelligence for healthcare payer refers to the use of artificial intelligence technologies to optimize administrative, financial, and clinical decision-making processes within health insurance and payer organizations. Its primary purpose is to improve claims processing, detect fraud, enhance member engagement, and support cost-effective, data-driven care management. The main components of artificial intelligence for healthcare payer are software and services. Software refers to AI-driven applications that automate claims, detect fraud, predict risks, and enhance decision-making to improve payer efficiency and cost management. It is powered by technologies such as machine learning (ML), natural language processing (NLP), and others and is deployed through cloud and on-premises modes. It finds applications in claims processing optimization, fraud detection and prevention, revenue management and billing, member engagement and personalization, risk adjustment and predictive analytics, administrative workflow automation, and others.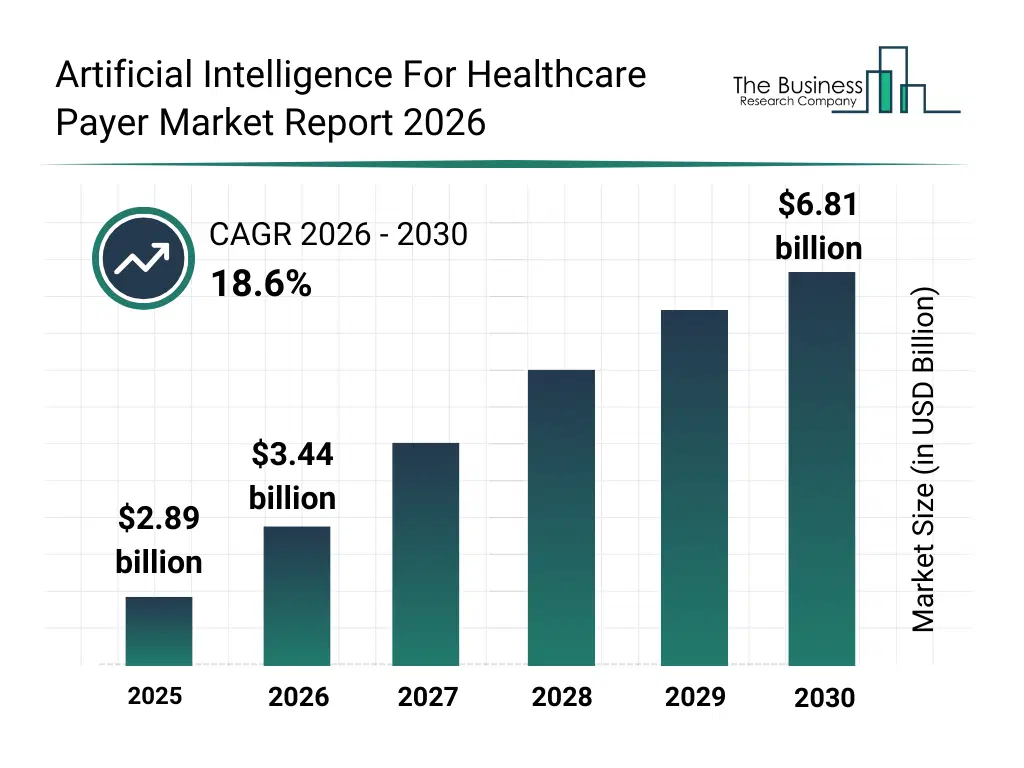
What Is The Artificial Intelligence For Healthcare Payer Market Size and Share 2026?
The artificial intelligence for healthcare payer market size has grown rapidly in recent years. It will grow from $2.89 billion in 2025 to $3.44 billion in 2026 at a compound annual growth rate (CAGR) of 18.9%. The growth in the historic period can be attributed to rising healthcare claims volumes, increasing complexity of reimbursement processes, growth of digital health data availability, early adoption of analytics-driven payer platforms, increasing pressure to reduce administrative costs.What Is The Artificial Intelligence For Healthcare Payer Market Growth Forecast?
The artificial intelligence for healthcare payer market size is expected to see rapid growth in the next few years. It will grow to $6.81 billion in 2030 at a compound annual growth rate (CAGR) of 18.6%. The growth in the forecast period can be attributed to increasing shift toward value-based care models, rising investments in cloud-based payer solutions, growing focus on predictive risk adjustment, expansion of ai-driven member personalization, increasing regulatory emphasis on fraud prevention. Major trends in the forecast period include increasing adoption of AI-based claims automation platforms, rising use of fraud detection and risk analytics tools, growing deployment of predictive cost management solutions, expansion of personalized member engagement systems, enhanced focus on administrative workflow optimization.Global Artificial Intelligence For Healthcare Payer Market Segmentation
1) By Component: Software, Services 2) By Technology: Machine Learning (ML), Natural Language Processing (NLP), Other Technologies 3) By Deployment: Cloud, On-Premises 4) By Application: Claims Processing Optimization, Fraud Detection and Prevention, Revenue Management and Billing, Member Engagement and Personalization, Risk Adjustment And Predictive Analytics, Administrative Workflow Automation, Other Applications Subsegments: 1) By Software: Predictive Analytics Platforms, Claims Management Solutions, Fraud Detection Systems, Risk Assessment Tools, Member Engagement Solutions 2) By Services: Implementation And Integration Services, Consulting Services, Support And Maintenance Services, Training And Education Services, Managed ServicesWhat Is The Driver Of The Artificial Intelligence For Healthcare Payer Market?
The growing volume of healthcare data is expected to propel the growth of artificial intelligence for the healthcare payer market going forward. Healthcare data refers to any information related to the health status, medical history, treatment, and healthcare services provided to individuals or populations. The growing volume of healthcare data is driven by digitalization, as electronic health records and connected devices enable faster, more accurate collection and analysis of patient information. Artificial intelligence (AI) for healthcare payers leverages the growing volume of healthcare data by utilizing vast datasets from electronic health records, claims, and wearable devices. It enhances decision-making through data-driven insights, enabling accurate risk assessment, fraud detection, and efficient claims management. For instance, in June 2022, according to the Department of Health and Social Care, a UK-based government department, 90% of National Health Service (NHS) trusts have adopted using electronic health records by December 2023 and are projected to reach 100% by March 2025. Therefore, the growing volume of healthcare data is driving the growth of artificial intelligence for the healthcare payer market.Key Players In The Global Artificial Intelligence For Healthcare Payer Market
Major companies operating in the artificial intelligence for healthcare payer market are Amazon Web Services Inc., Google LLC, Microsoft Corporation, Accenture plc, Oracle Corporation, Cognizant Technology Solutions Corporation, Wipro Limited, SAS Institute Inc., Hexaware Technologies Limited, Firstsource Solutions Limited, Innovaccer Incorporated, Cohere Health Incorporated, Softheon, MST Solutions LLC, Lyric AI Incorporated, Inovaare Corporation, Codoxo, Iatros Health Incorporated, Optum Inc., Cerner CorporationGlobal Artificial Intelligence For Healthcare Payer Market Trends and Insights
Major companies operating in the artificial intelligence for healthcare payer market are focusing on developing advanced digital solutions, such as AI-powered patient navigation tools, to boost efficiency, enhance member experience, and reduce administrative burdens. Artificial intelligence (AI)-powered patient navigation tools refer to advanced digital systems that use artificial intelligence to help patients understand their benefits, find in-network care, and estimate costs. For instance, in April 2024, CVS Health Corporation, a US-based health solutions company, launched a suite of new AI and digital tools. These tools include an AI-powered member experience designed to simplify finding in-network care and understanding costs. It features a personalized patient navigation tool that guides members to the most appropriate site of care such as primary care, urgent care, or a specialist based on their symptoms, benefits, and local availability, enabling seamless access to care with reduced effort.What Are Latest Mergers And Acquisitions In The Artificial Intelligence For Healthcare Payer Market?
In September 2025, Cohere Health Inc., a US-based healthcare technology company, acquired ZignaAI Inc. for an undisclosed amount. With this acquisition, Cohere Health aims to enhance its AI-driven payment integrity and revenue optimization capabilities, enabling health plans to automate claims validation, improve pricing accuracy, and strengthen overall payer operational efficiency. ZignaAI Inc. is a US-based artificial intelligence (AI) company specializing in payment integrity and revenue optimization solutions for healthcare payers.Regional Outlook
North America was the largest region in the artificial intelligence for healthcare payer market in 2025. Asia-Pacific is expected to be the fastest-growing region in the forecast period. The regions covered in this market report are Asia-Pacific, South East Asia, Western Europe, Eastern Europe, North America, South America, Middle East, Africa. The countries covered in this market report are Australia, Brazil, China, France, Germany, India, Indonesia, Japan, Taiwan, Russia, South Korea, UK, USA, Canada, Italy, Spain.What Defines the Artificial Intelligence For Healthcare Payer Market?
The artificial intelligence for healthcare payer market consists of revenues earned by entities by providing services such as data analytics, predictive modeling, patient engagement, prior authorization automation, healthcare data integration, and clinical decision support services. The market value includes the value of related goods sold by the service provider or included within the service offering. The artificial intelligence for healthcare payer also includes sales of automated claims processing systems, predictive risk modeling software, healthcare data management systems, clinical decision support tools, fraud detection devices, AI-driven chatbots, data storage servers, and workflow automation tools. Values in this market are ‘factory gate’ values, that is the value of goods sold by the manufacturers or creators of the goods, whether to other entities (including downstream manufacturers, wholesalers, distributors and retailers) or directly to end customers. The value of goods in this market includes related services sold by the creators of the goods.How is Market Value Defined and Measured?
The market value is defined as the revenues that enterprises gain from the sale of goods and/or services within the specified market and geography through sales, grants, or donations in terms of the currency (in USD unless otherwise specified). The revenues for a specified geography are consumption values that are revenues generated by organizations in the specified geography within the market, irrespective of where they are produced. It does not include revenues from resales along the supply chain, either further along the supply chain or as part of other products.What Key Data and Analysis Are Included in the Artificial Intelligence For Healthcare Payer Market Report 2026?
The artificial intelligence for healthcare payer market research report is one of a series of new reports from The Business Research Company that provides market statistics, including industry global market size, regional shares, competitors with the market share, detailed market segments, market trends and opportunities, and any further data you may need to thrive in the artificial intelligence for healthcare payer industry. The market research report delivers a complete perspective of everything you need, with an in-depth analysis of the current and future state of the industry.Artificial Intelligence For Healthcare Payer Market Report Forecast Analysis
| Report Attribute | Details |
|---|---|
| Market Size Value In 2026 | $3.44 billion |
| Revenue Forecast In 2035 | $6.81 billion |
| Growth Rate | CAGR of 18.9% from 2026 to 2035 |
| Base Year For Estimation | 2025 |
| Actual Estimates/Historical Data | 2020-2025 |
| Forecast Period | 2026 - 2030 - 2035 |
| Market Representation | Revenue in USD Billion and CAGR from 2026 to 2035 |
| Segments Covered | Component, Technology, Deployment, Application |
| Regional Scope | Asia-Pacific, Western Europe, Eastern Europe, North America, South America, Middle East, Africa |
| Country Scope | The countries covered in the report are Australia, Brazil, China, France, Germany, India, ... |
| Key Companies Profiled | Amazon Web Services Inc., Google LLC, Microsoft Corporation, Accenture plc, Oracle Corporation, Cognizant Technology Solutions Corporation, Wipro Limited, SAS Institute Inc., Hexaware Technologies Limited, Firstsource Solutions Limited, Innovaccer Incorporated, Cohere Health Incorporated, Softheon, MST Solutions LLC, Lyric AI Incorporated, Inovaare Corporation, Codoxo, Iatros Health Incorporated, Optum Inc., Cerner Corporation |
| Customization Scope | Request for Customization |
| Pricing And Purchase Options | Explore Purchase Options |
Frequently Asked Questions
The Artificial Intelligence For Healthcare Payer market was valued at $2.89 billion in 2025, increased to $3.44 billion in 2026, and is projected to reach $6.81 billion by 2030.
The global Artificial Intelligence For Healthcare Payer market is expected to grow at a CAGR of 18.6% from 2026 to 2035 to reach $6.81 billion by 2035.
Some Key Players in the Artificial Intelligence For Healthcare Payer market Include, Amazon Web Services Inc., Google LLC, Microsoft Corporation, Accenture plc, Oracle Corporation, Cognizant Technology Solutions Corporation, Wipro Limited, SAS Institute Inc., Hexaware Technologies Limited, Firstsource Solutions Limited, Innovaccer Incorporated, Cohere Health Incorporated, Softheon, MST Solutions LLC, Lyric AI Incorporated, Inovaare Corporation, Codoxo, Iatros Health Incorporated, Optum Inc., Cerner Corporation .
Major trend in this market includes: AI-Powered Platform Improves Efficiency And Reduces Burden. For further insights on this market.
Request for SampleNorth America was the largest region in the artificial intelligence for healthcare payer market in 2025. Asia-Pacific is expected to be the fastest-growing region in the forecast period. The regions covered in the artificial intelligence for healthcare payer market report are Asia-Pacific, South East Asia, Western Europe, Eastern Europe, North America, South America, Middle East, Africa.
