
Healthcare Claims Management Solutions Market Report 2026
Global Outlook – By Type (Software, Services), By Deployment Mode (Web-Based, Cloud-Based, On-Premise), By End-User (Healthcare Payers, Healthcare Providers, Other End-Users) - Market Size, Trends, And Global Forecast 2026-2035
Healthcare Claims Management Solutions Market Overview
• Healthcare Claims Management Solutions market size has reached to $17.43 billion in 2025 • Expected to grow to $24.47 billion in 2030 at a compound annual growth rate (CAGR) of 7% • Growth Driver: Rising Chronic Disease Cases Fuel Growth In Healthcare Claims Management Market • Market Trend: Technological Advancement Revolutionizes The Healthcare Claims Management Solutions Market • North America was the largest region in 2025 and Asia-Pacific is the fastest growing region.What Is Covered Under Healthcare Claims Management Solutions Market?
Healthcare claims management solutions refer to solutions that strive to provide complete automation of claims processing and speedier access to client information while maintaining the protection of private medical information. The main types of healthcare claims management solutions are software and services. Software refers to a set of data, instructions, or programs that are used in computers to complete specific tasks. These are deployed through web-based, cloud-based, and on-premise deployment. The various end-users include healthcare payers, healthcare providers, and other end-users.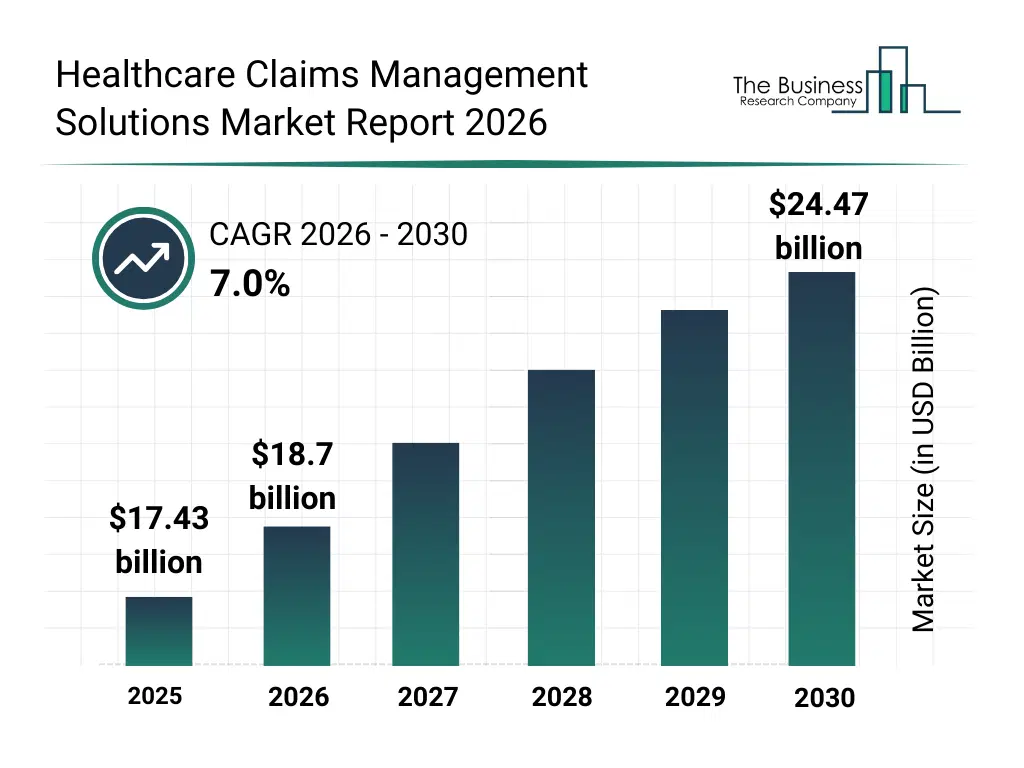
What Is The Healthcare Claims Management Solutions Market Size and Share 2026?
The healthcare claims management solutions market size has grown strongly in recent years. It will grow from $17.43 billion in 2025 to $18.7 billion in 2026 at a compound annual growth rate (CAGR) of 7.3%. The growth in the historic period can be attributed to increasing healthcare insurance coverage, rising claim volumes across providers, adoption of digital billing systems, growing complexity of reimbursement processes, demand for faster claim settlement.What Is The Healthcare Claims Management Solutions Market Growth Forecast?
The healthcare claims management solutions market size is expected to see strong growth in the next few years. It will grow to $24.47 billion in 2030 at a compound annual growth rate (CAGR) of 7.0%. The growth in the forecast period can be attributed to increasing deployment of AI-driven claims platforms, rising focus on value-based care reimbursement, expansion of cloud-based claims solutions, growing emphasis on regulatory compliance automation, demand for real-time claims transparency. Major trends in the forecast period include increasing adoption of automated claims processing systems, rising use of predictive analytics for claims accuracy, growing integration of real-time patient data access, expansion of fraud detection and prevention tools, enhanced focus on data security and compliance.Global Healthcare Claims Management Solutions Market Segmentation
1) By Type: Software, Services 2) By Deployment Mode: Web-Based, Cloud-Based, On-Premise 3) By End-User: Healthcare Payers, Healthcare Providers, Other End-Users Subsegments: 1) By Software: Claims Processing Software, Revenue Cycle Management Software, Medical Billing Software, Analytics And Reporting Tools 2) By Services: Consulting Services, Implementation Services, Training And Support Services, Claims Auditing ServicesWhat Is The Driver Of The Healthcare Claims Management Solutions Market?
The increasing incidence of chronic diseases is expected to propel the growth of healthcare claims management solutions market going forward. Chronic diseases refer to long-lasting health conditions that persist over an extended period and typically require ongoing medical management. Healthcare claims management solutions are used as crucial support for the efficient and accurate processing of claims, ensuring that healthcare providers receive timely reimbursement for chronic disease management services. For instance, in January 2023, according to the National Center for Biotechnology Information (NCBI), a US-based National Library of Medicine, it is projected that by the year 2050, the number of individuals aged 50 years and older who have at least one chronic illness will surge by 99.5%, rising to 142.66 million. Therefore, the increasing incidence of chronic diseases will propel the healthcare claims management solutions industry.Key Players In The Global Healthcare Claims Management Solutions Market
Major companies operating in the healthcare claims management solutions market are Allscripts Healthcare Solutions Inc, Athenahealth, McKesson Corporation, Oracle Corporation, Availity LLC, Cerner Corporation, Change Healthcare, Conifer Health Solutions LLC, eClinicalWorks, Emdeon Inc, Epic Systems Corporation, Inovalon Co, InstaMed LLC, Kareo Co, NaviNet Inc, NTT Data Services, Optum Inc, SSI Group LLC, Cognizant Technology Ltd, TruBridge Co, Waystar Co, ZirMed IncGlobal Healthcare Claims Management Solutions Market Trends and Insights
Major companies operating in the healthcare claims management solutions market are focusing on product innovation such as the AI-enabled claims data activator Suite to sustain their position in the market. Claims Data Activator establishes data interoperability, intelligent analytics, and smart reporting by using Document AI, the Healthcare Natural Language API, and the Healthcare API to convert unstructured data to structured data. For instance, in April 2023, Google LLC, a US-based technology company, launched a new Google Cloud AI-enabled claims data activator that will assist health plans and providers in lowering administrative costs and responsibilities by transforming unstructured data into structured data and empowering specialists to make quicker, better-informed decisions that enhance patient care.What Are Latest Mergers And Acquisitions In The Healthcare Claims Management Solutions Market?
In July 2024, Medlogix, LLC, a US-based provider of technology-driven, clinically based medical claims‑management services, acquired ReviewWorks for an undisclosed amount. With this acquisition, Medlogix aimed to bolster its clinical cost‑containment and disability-management capabilities by combining ReviewWorks’ specialized medical review services with its claims management platform. ReviewWorks is a US-based provider of medical cost-containment solutions and claim management solution.Regional Outlook
North America was the largest region in the healthcare claim management solution market in 2025. Asia-Pacific is expected to be the fastest-growing region in the forecast period. The regions covered in this market report are Asia-Pacific, South East Asia, Western Europe, Eastern Europe, North America, South America, Middle East, Africa. The countries covered in this market report are Australia, Brazil, China, France, Germany, India, Indonesia, Japan, Taiwan, Russia, South Korea, UK, USA, Canada, Italy, Spain.What Defines the Healthcare Claims Management Solutions Market?
The healthcare claims management solutions market consists of sales of healthcare software and related services. Values in this market are ‘factory gate’ values, that is the value of goods sold by the manufacturers or creators of the goods, whether to other entities (including downstream manufacturers, wholesalers, distributors and retailers) or directly to end customers. The value of goods in this market includes related services sold by the creators of the goods.How is Market Value Defined and Measured?
The market value is defined as the revenues that enterprises gain from the sale of goods and/or services within the specified market and geography through sales, grants, or donations in terms of the currency (in USD unless otherwise specified). The revenues for a specified geography are consumption values that are revenues generated by organizations in the specified geography within the market, irrespective of where they are produced. It does not include revenues from resales along the supply chain, either further along the supply chain or as part of other products.What Key Data and Analysis Are Included in the Healthcare Claims Management Solutions Market Report 2026?
The healthcare claims management solutions market research report is one of a series of new reports from The Business Research Company that provides market statistics, including industry global market size, regional shares, competitors with the market share, detailed market segments, market trends and opportunities, and any further data you may need to thrive in the healthcare claims management solutions industry. The market research report delivers a complete perspective of everything you need, with an in-depth analysis of the current and future state of the industry.Healthcare Claims Management Solutions Market Report Forecast Analysis
| Report Attribute | Details |
|---|---|
| Market Size Value In 2026 | $18.7 billion |
| Revenue Forecast In 2035 | $24.47 billion |
| Growth Rate | CAGR of 7.3% from 2026 to 2035 |
| Base Year For Estimation | 2025 |
| Actual Estimates/Historical Data | 2020-2025 |
| Forecast Period | 2026 - 2030 - 2035 |
| Market Representation | Revenue in USD Billion and CAGR from 2026 to 2035 |
| Segments Covered | Type, Deployment Mode, End-User |
| Regional Scope | Asia-Pacific, Western Europe, Eastern Europe, North America, South America, Middle East, Africa |
| Country Scope | The countries covered in the report are Australia, Brazil, China, France, Germany, India, ... |
| Key Companies Profiled | Allscripts Healthcare Solutions Inc, Athenahealth, McKesson Corporation, Oracle Corporation, Availity LLC, Cerner Corporation, Change Healthcare, Conifer Health Solutions LLC, eClinicalWorks, Emdeon Inc, Epic Systems Corporation, Inovalon Co, InstaMed LLC, Kareo Co, NaviNet Inc, NTT Data Services, Optum Inc, SSI Group LLC, Cognizant Technology Ltd, TruBridge Co, Waystar Co, ZirMed Inc |
| Customization Scope | Request for Customization |
| Pricing And Purchase Options | Explore Purchase Options |
