
Healthcare Fraud Analytics Market Report 2026
Global Outlook – By Solution Type (Descriptive Analytics, Predictive Analytics, Prescriptive Analytics), By Delivery Model (On-Premise, On-Demand), By Application (Insurance Claims Review, Postpayment Review, Prepayment Review, Pharmacy Billing Misuse, Payment Integrity, Other Applications) – Market Size, Trends, Strategies, and Forecast to 2035
Healthcare Fraud Analytics Market Overview
• Healthcare Fraud Analytics market size has reached to $4.65 billion in 2025 • Expected to grow to $15.37 billion in 2030 at a compound annual growth rate (CAGR) of 26.9% • Growth Driver: Rise In Fraudulent Activities In The Healthcare Sector Drives The Healthcare Fraud Analytics Market • Market Trend: Rising Technological Advancements Transforming Healthcare Fraud Analytics Market • North America was the largest region and fastest growing region.What Is Covered Under Healthcare Fraud Analytics Market?
Healthcare fraud analytics refers to on-premise and on-demand analytical solutions that assist in identifying issues such as duplication/repetition of claims and errors in claim healthcare operations and applications. Healthcare fraud analytics aims to help healthcare companies to audit their accounts and find out fraudulent activities in various transactions. It identifies frauds related to billings, claims, prepayment, post payments, and payment integrity. The main type of solutions in healthcare fraud analytics are descriptive analytics, predictive analytics, prescriptive analytics. Descriptive analytics is a process of using current and historical data to identify trends and relationships. Healthcare fraud analytic solutions are deployed on-premise and on-demand, and they are widely used for insurance claims review, postpayment review, prepayment review, pharmacy billing misuse, payment integrity, and other applications. Healthcare fraud analytics are used by public & government agencies, private insurance payers, third-party service providers.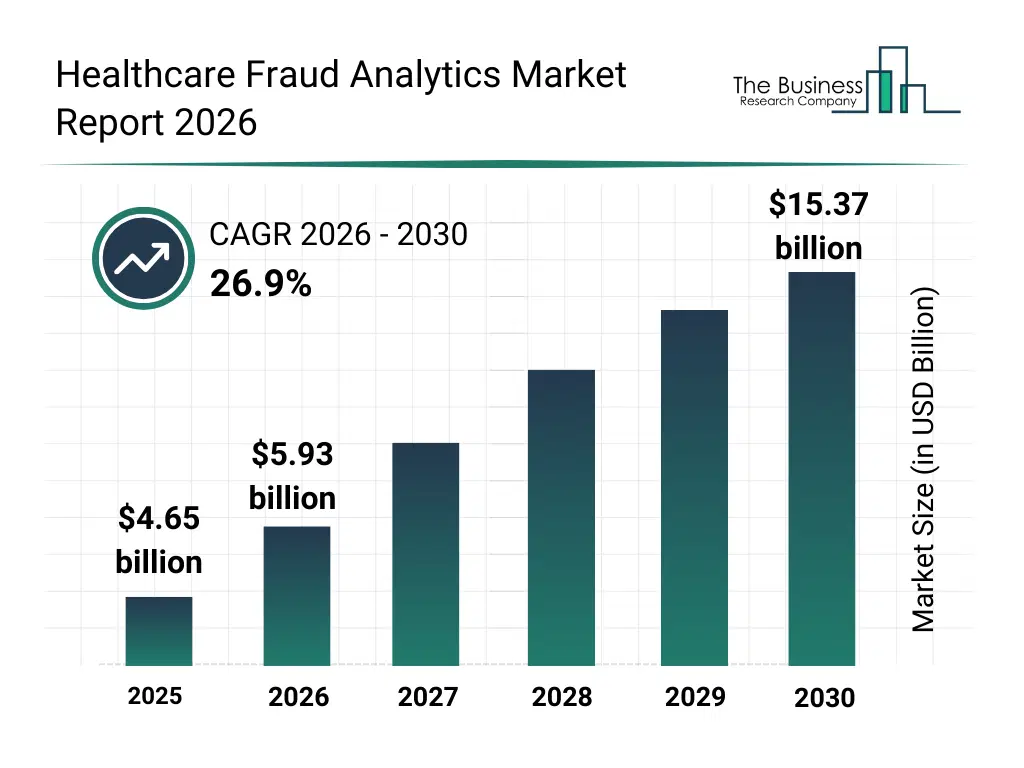
What Is The Healthcare Fraud Analytics Market Size and Share 2026?
The healthcare fraud analytics market size has grown exponentially in recent years. It will grow from $4.65 billion in 2025 to $5.93 billion in 2026 at a compound annual growth rate (CAGR) of 27.5%. The growth in the historic period can be attributed to increasing healthcare claim volumes, rising complexity of billing processes, growth in digital healthcare transactions, expansion of insurance coverage programs, availability of healthcare data analytics tools.What Is The Healthcare Fraud Analytics Market Growth Forecast?
The healthcare fraud analytics market size is expected to see exponential growth in the next few years. It will grow to $15.37 billion in 2030 at a compound annual growth rate (CAGR) of 26.9%. The growth in the forecast period can be attributed to increasing investments in advanced fraud prevention platforms, rising regulatory scrutiny on healthcare payments, expansion of machine learning-based analytics, growing adoption of cloud-based fraud solutions, increasing focus on cost containment in healthcare. Major trends in the forecast period include increasing use of predictive fraud detection models, rising adoption of real-time claims analytics, growing integration of ai-driven anomaly detection, expansion of automated payment integrity solutions, enhanced focus on prepayment fraud prevention.Global Healthcare Fraud Analytics Market Segmentation
1) By Solution Type: Descriptive Analytics, Predictive Analytics, Prescriptive Analytics 2) By Delivery Model: On-Premise, On-Demand 3) By Application: Insurance Claims Review, Postpayment Review, Prepayment Review, Pharmacy Billing Misuse, Payment Integrity, Other Applications Subsegments: 1) By Descriptive Analytics: Data Aggregation, Reporting Tools, Visualization Techniques 2) By Predictive Analytics: Risk Assessment Models, Trend analysis, Anomaly Detection 3) By Prescriptive Analytics: Recommendation Engines, Simulation Models, Resource Allocation ToolsWhat Is The Driver Of The Healthcare Fraud Analytics Market?
A large number of fraudulent activities in the healthcare sector contribute to the growth of the healthcare fraud analytics market. Medical providers, patients, and third parties who intentionally deceive the healthcare system into acquiring unlawful benefits can commit fraud based on deception or misrepresentation. These frauds and abuses involve kickbacks, billing, billing for services not provided, medical testing, and other fraudulent activities. For instance, in December 2023, the U.S. Department of Health and Human Services (HHS) reported that healthcare fraud investigations resulted in recoveries totaling over $1.72 billion. The majority of these recoveries, approximately $1.2 billion, were returned to the Medicare Trust Funds. Additionally, the Department of Justice (DOJ) reported that in fiscal year 2023, settlements and judgments under the False Claims Act exceeded $2.68 billion, indicating a strong enforcement response to fraudulent practices. These figures reflect the significant financial impact of healthcare fraud, which is estimated to cost the nation billions annually, with some estimates suggesting losses could be as high as 10% of annual healthcare expenditure. Thus, the increasing number of fraudulent activities in healthcare is contributing to the healthcare fraud market growth.Key Players In The Global Healthcare Fraud Analytics Market
Major companies operating in the healthcare fraud analytics market are International Business Machines Corporation; Optum Inc.; Statistical Analysis Software Institute Inc.; Change Healthcare; EXL Service Holdings Inc.; Cotiviti Inc.; DXC Technology Company; Wipro Limited; Conduent Incorporated; HCL Technologies Limited; Qlarant Inc.; LEXIS-NEXIS Group; Healthcare Fraud Shield; FraudLens Inc.; HMS Holding Corp.; Codoxo; H20. ai; Pondera Solutions Inc.; Friss International B. V.; MultiPlan Inc.; FraudScope; Osp Labs Private Limited; Fair Isaac Corporation; Relx Group PLCGlobal Healthcare Fraud Analytics Market Trends and Insights
Major players in the healthcare fraud analytics market are focusing on investments to expand in the market. Rising technological advancements in healthcare fraud analytics denote the increasing allocation of financial resources towards advanced analytical tools and technologies aimed at detecting and preventing fraudulent activities within the healthcare sector. For instance, in August 2024, MediBuddy, an India-based digital healthcare company, launched an innovative AI-powered fraud detection system named Sherlock aimed at combating healthcare fraud, particularly in the realm of medical reimbursement claims. This advanced platform utilizes cutting-edge artificial intelligence (AI) and machine learning (ML) technologies to identify and prevent fraudulent activities in real-time, thereby enhancing the integrity of the healthcare system.What Are Latest Mergers And Acquisitions In The Healthcare Fraud Analytics Market?
In August 2024, Experian, an Ireland-based business services company, acquired NeuroID for an undisclosed amount. With this acquisition, Experian aims to enhance its identity verification and fraud prevention capabilities by integrating NeuroID's behavioral analytics technology, allowing for deeper insights into consumer behavior and improved detection of fraudulent activities across digital interactions. NeuroID is a US-based software company that offers healthcare fraud analytics.Regional Insights
North America was the largest region in the healthcare fraud analytics market in 2025.North America is expected to be the fastest-growing region in the forecast period. The regions covered in this market report are Asia-Pacific, South East Asia, Western Europe, Eastern Europe, North America, South America, Middle East, Africa. The countries covered in this market report are Australia, Brazil, China, France, Germany, India, Indonesia, Japan, Taiwan, Russia, South Korea, UK, USA, Canada, Italy, SpainWhat Defines the Healthcare Fraud Analytics Market?
The healthcare fraud analytics market includes revenues earned by entities by providing services such as fraud detection, predictive analytics, and Medicaid. The market value includes the value of related goods sold by the service provider or included within the service offering. Only goods and services traded between entities or sold to end consumers are included.How is Market Value Defined and Measured?
The market value is defined as the revenues that enterprises gain from the sale of goods and/or services within the specified market and geography through sales, grants, or donations in terms of the currency (in USD unless otherwise specified). The revenues for a specified geography are consumption values that are revenues generated by organizations in the specified geography within the market, irrespective of where they are produced. It does not include revenues from resales along the supply chain, either further along the supply chain or as part of other products.What Key Data and Analysis Are Included in the Healthcare Fraud Analytics Market Report 2026?
The healthcare fraud analytics market research report is one of a series of new reports from The Business Research Company that provides market statistics, including industry global market size, regional shares, competitors with the market share, detailed market segments, market trends and opportunities, and any further data you may need to thrive in the healthcare fraud analytics industry. The market research report delivers a complete perspective of everything you need, with an in-depth analysis of the current and future state of the industry.Healthcare Fraud Analytics Market Report Forecast Analysis
| Report Attribute | Details |
|---|---|
| Market Size Value In 2026 | $5.93 billion |
| Revenue Forecast In 2035 | $15.37 billion |
| Growth Rate | CAGR of 27.5% from 2026 to 2035 |
| Base Year For Estimation | 2025 |
| Actual Estimates/Historical Data | 2020-2025 |
| Forecast Period | 2026 - 2030 - 2035 |
| Market Representation | Revenue in USD Billion and CAGR from 2026 to 2035 |
| Segments Covered | Solution Type, Delivery Model, Application |
| Regional Scope | Asia-Pacific, Western Europe, Eastern Europe, North America, South America, Middle East, Africa |
| Country Scope | The countries covered in the report are Australia, Brazil, China, France, Germany, India, ... |
| Key Companies Profiled | International Business Machines Corporation; Optum Inc.; Statistical Analysis Software Institute Inc.; Change Healthcare; EXL Service Holdings Inc.; Cotiviti Inc.; DXC Technology Company; Wipro Limited; Conduent Incorporated; HCL Technologies Limited; Qlarant Inc.; LEXIS-NEXIS Group; Healthcare Fraud Shield; FraudLens Inc.; HMS Holding Corp.; Codoxo; H20. ai; Pondera Solutions Inc.; Friss International B. V.; MultiPlan Inc.; FraudScope; Osp Labs Private Limited; Fair Isaac Corporation; Relx Group PLC |
| Customization Scope | Request for Customization |
| Pricing And Purchase Options | Explore Purchase Options |
