
Healthcare Provider Network Management Market Report 2026
Global Outlook – By Component (Network Management Services, Network Management Software ), By Deployment Type (On-Premises, Cloud ), By End User (Private Payers, Public Payers) - Market Size, Trends, And Global Forecast 2026-2035
Healthcare Provider Network Management Market Overview
• Healthcare Provider Network Management market size has reached to $5.52 billion in 2025 • Expected to grow to $11.51 billion in 2030 at a compound annual growth rate (CAGR) of 15.7% • Growth Driver: Increasing Geriatric Population And Healthcare Provider Network Management • Market Trend: Advancements in Healthcare Provider Network Management • North America was the largest region in 2025.What Is Covered Under Healthcare Provider Network Management Market?
Healthcare provider network management provides a point for access to information about health insurance plans, government regulations and processes, pricing, and other data within the healthcare organization. The main types of components in the healthcare provider network management market are network management services and network management software. The network management services market refers to services used to provide access to plans of patient care, pathology report results, and medical and pharmacy claims utilization data. The network management services refer to network maintenance, monitoring of devices, and monthly report status. The various deployment types include on-premises and cloud, and the end users are private payers and public payers.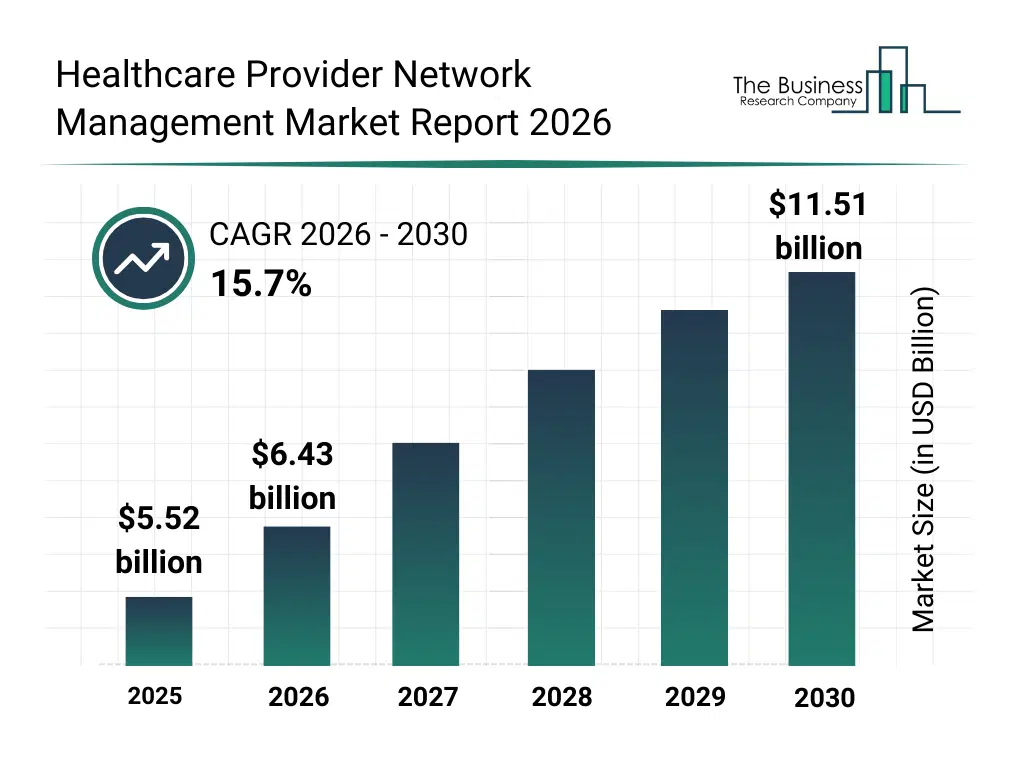
What Is The Healthcare Provider Network Management Market Size and Share 2026?
The healthcare provider network management market size has grown rapidly in recent years. It will grow from $5.52 billion in 2025 to $6.43 billion in 2026 at a compound annual growth rate (CAGR) of 16.4%. The growth in the historic period can be attributed to growing complexity of provider networks, increasing demand for accurate credentialing processes, expansion of managed care organizations, rising compliance documentation needs, adoption of digital provider directories.What Is The Healthcare Provider Network Management Market Growth Forecast?
The healthcare provider network management market size is expected to see rapid growth in the next few years. It will grow to $11.51 billion in 2030 at a compound annual growth rate (CAGR) of 15.7%. The growth in the forecast period can be attributed to increasing shift toward value-based reimbursement models, rising investments in provider analytics platforms, growing demand for real-time network visibility, expansion of cloud deployments, increasing focus on cost and quality optimization. Major trends in the forecast period include increasing adoption of centralized provider data platforms, rising use of credentialing automation tools, growing focus on network performance analytics, expansion of cloud-based network management systems, enhanced integration of contract management solutions.Global Healthcare Provider Network Management Market Segmentation
1) By Component: Network Management Services, Network Management Software 2) By Deployment Type: On-Premises, Cloud 3) By End User: Private Payers, Public Payers Subsegments: 1) By Network Management Services: Provider Enrollment Services, Credentialing And Privileging Services, Network Development And Optimization Services, Performance Analytics And Reporting Services, Contract Management Services 2) By Network Management Software: Provider Network Management Software, Data Analytics And Reporting Tools, Credentialing Software, Contract Management SystemsWhat Is The Driver Of The Healthcare Provider Network Management Market?
The increasing geriatric population is expected to propel the growth of the healthcare provider network management market going forward. The geriatric population refers to individuals who are elderly, typically aged 65 and older, characterized by specific healthcare needs associated with aging. The Healthcare Provider Network Management market plays a pivotal role in addressing the evolving needs of an increasing geriatric population by optimizing healthcare delivery, enhancing care coordination, and ensuring efficient resource allocation. As the demographic landscape shifts towards a larger elderly population, effective network management becomes a strategic imperative to meet the unique healthcare demands of this growing segment. For instance, in July 2024, according to the UK Parliament's House of Commons Library, a UK-based government administration, in 2022, there were 12.7 million individuals aged 65 and older in the UK, accounting for 19% of the total population. This number is projected to rise to 22.1 million by 2072, representing 27% of the population. Therefore, the increasing geriatric population is driving the growth of the healthcare provider network management industry.Key Players In The Global Healthcare Provider Network Management Market
Major companies operating in the healthcare provider network management market are UnitedHealth Group Incorporated, Cigna Corporation, Elevance Health Inc., Humana Inc., Centene Corporation, CVS Health Corporation, Molina Healthcare Inc., GuideWell Mutual Holding Corporation, Blue Cross Blue Shield Association, Kaiser Permanente, Highmark Health, CareSource, Independence Health Group, UPMC Health Plan, Oscar Health, SCAN Health Plan, WellCare Health Plans, Bupa Group, AXA Group, Allianz SE, UnitedHealthcare Community PlanGlobal Healthcare Provider Network Management Market Trends and Insights
Major companies operating in the healthcare provider network management market are focusing on introducing advanced products such as ICU on wheels to gain competitive edge. ICU on wheels refers to a mobile intensive care unit designed to provide critical medical care and advanced life support to patients while transporting them, often used in emergencies or during patient transfers between facilities. For instance, in November 2023, HealthNet, is an US based health care insurance provider, launched 5G ambulance, equipped with real-time data transmission and advanced medical technology. This vehicle enables seamless communication between paramedics and hospitals, allowing critical patient data to be transmitted instantly, enhancing emergency care response. By integrating into the broader healthcare provider network, the 5G ambulance improves decision-making and patient outcomes, reinforcing HealthNet’s role in advancing provider network management.What Are Latest Mergers And Acquisitions In The Healthcare Provider Network Management Market?
In January 2025, Innovaccer, a US-based healthcare technology company, acquired Humbi AI, for an undisclosed amount. With this acquisition, Innovaccer aims to launch actuarial and contracting copilot capabilities for payers, providers, and life sciences companies, enhancing its AI-driven healthcare solutions and streamlining decision-making processes. Humbi AI is a US-based an actuarial intelligence company specializing in AI-powered tools for healthcare analytics and contract management.Regional Outlook
North America was the largest region in the healthcare provider network management market in 2025. The regions covered in this market report are Asia-Pacific, South East Asia, Western Europe, Eastern Europe, North America, South America, Middle East, Africa. The countries covered in this market report are Australia, Brazil, China, France, Germany, India, Indonesia, Japan, Taiwan, Russia, South Korea, UK, USA, Canada, Italy, Spain.What Defines the Healthcare Provider Network Management Market?
The healthcare provider network management market includes revenues earned by software and services. The market value includes the value of related goods sold by the service provider or included within the service offering. Only goods and services traded between entities or sold to end consumers are included.How is Market Value Defined and Measured?
The market value is defined as the revenues that enterprises gain from the sale of goods and/or services within the specified market and geography through sales, grants, or donations in terms of the currency (in USD unless otherwise specified). The revenues for a specified geography are consumption values that are revenues generated by organizations in the specified geography within the market, irrespective of where they are produced. It does not include revenues from resales along the supply chain, either further along the supply chain or as part of other products.What Key Data and Analysis Are Included in the Healthcare Provider Network Management Market Report 2026?
The healthcare provider network management market research report is one of a series of new reports from The Business Research Company that provides market statistics, including industry global market size, regional shares, competitors with the market share, detailed market segments, market trends and opportunities, and any further data you may need to thrive in the healthcare provider network management industry. The market research report delivers a complete perspective of everything you need, with an in-depth analysis of the current and future state of the industry.Healthcare Provider Network Management Market Report Forecast Analysis
| Report Attribute | Details |
|---|---|
| Market Size Value In 2026 | $6.43 billion |
| Revenue Forecast In 2035 | $11.51 billion |
| Growth Rate | CAGR of 16.4% from 2026 to 2035 |
| Base Year For Estimation | 2025 |
| Actual Estimates/Historical Data | 2020-2025 |
| Forecast Period | 2026 - 2030 - 2035 |
| Market Representation | Revenue in USD Billion and CAGR from 2026 to 2035 |
| Segments Covered | Component, Deployment Type, End User |
| Regional Scope | Asia-Pacific, Western Europe, Eastern Europe, North America, South America, Middle East, Africa |
| Country Scope | The countries covered in the report are Australia, Brazil, China, France, Germany, India, ... |
| Key Companies Profiled | UnitedHealth Group Incorporated, Cigna Corporation, Elevance Health Inc., Humana Inc., Centene Corporation, CVS Health Corporation, Molina Healthcare Inc., GuideWell Mutual Holding Corporation, Blue Cross Blue Shield Association, Kaiser Permanente, Highmark Health, CareSource, Independence Health Group, UPMC Health Plan, Oscar Health, SCAN Health Plan, WellCare Health Plans, Bupa Group, AXA Group, Allianz SE, UnitedHealthcare Community Plan |
| Customization Scope | Request for Customization |
| Pricing And Purchase Options | Explore Purchase Options |
