
Pharmacy Benefit Management Market Report 2026
Global Outlook – By Services (Mail-Delivery, Specialty Pharmacy, Preferred Network Pharmacy), By Type (Commercial Health Plans, Self-Insured Employer Plans, Medicare Part D Plans, Federal Employees Health Benefits Program), By End User (Pharmacy Benefit Management Organization, Mail Order Pharmacies, Retail Pharmacies, Inpatient Pharmacies, Outpatient Pharmacies) - Market Size, Trends, And Global Forecast 2026-2035
Pharmacy Benefit Management Market Overview
• Pharmacy Benefit Management market size has reached to $695.73 billion in 2025 • Expected to grow to $1033.9 billion in 2030 at a compound annual growth rate (CAGR) of 8.2% • Growth Driver: Rising Chronic Disease Burden Accelerates Growth In Pharmacy Benefit Management Market • Market Trend: Innovations In Pharmacy Benefit Management Through Technology And Clinical Services • North America was the largest region in 2025 and Asia-Pacific is the fastest growing region.What Is Covered Under Pharmacy Benefit Management Market?
Pharmacy benefit management is a collection of businesses that function as intermediaries between insurance companies, pharmacies, and drug distributors. It is used to ensure that insurers and insurance companies pay reduced prescription costs by negotiating with pharmacists and medicine producers. The main services of the pharmacy benefit management (PBM) are mail-delivery, specialty pharmacy, and preferred network pharmacy. Mail-delivery refers to mail order delivery that directly delivers the medicines to the desired location. These services are provided for different types of PBM. The different types of PBMs are commercial health plans, self-insured employer plans, medicare part D plans, and federal employees health benefits program. These different PBMs cater to major end-users which include pharmacy benefit management organization, mail order pharmacies, retail pharmacies, inpatient pharmacies, and outpatient pharmacies.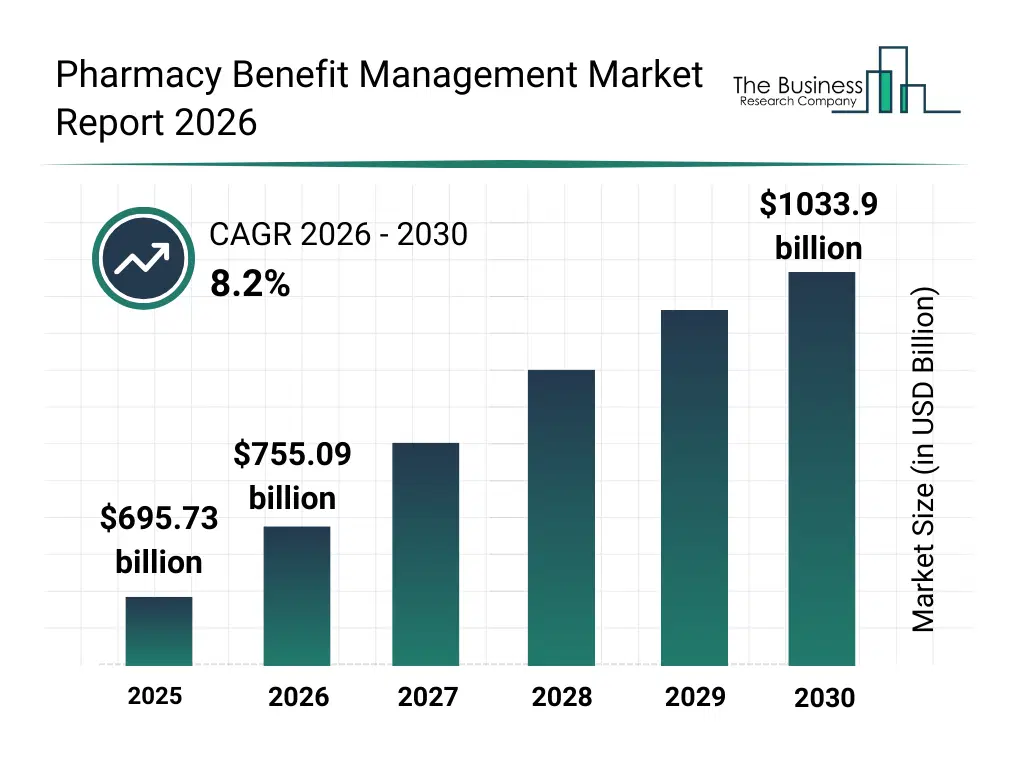
What Is The Pharmacy Benefit Management Market Size and Share 2026?
The pharmacy benefit management market size has grown strongly in recent years. It will grow from $695.73 billion in 2025 to $755.09 billion in 2026 at a compound annual growth rate (CAGR) of 8.5%. The growth in the historic period can be attributed to rising healthcare expenditure levels, expansion of insured populations, increasing complexity of drug pricing, early adoption of managed pharmacy networks, growth of mail-order pharmacy services.What Is The Pharmacy Benefit Management Market Growth Forecast?
The pharmacy benefit management market size is expected to see strong growth in the next few years. It will grow to $1033.9 billion in 2030 at a compound annual growth rate (CAGR) of 8.2%. The growth in the forecast period can be attributed to increasing use of AI-enabled cost optimization tools, rising focus on value-based care models, expansion of specialty drug management, growing regulatory scrutiny on drug pricing, increasing digitalization of pharmacy benefit platforms. Major trends in the forecast period include increasing adoption of data-driven formulary management, rising use of predictive cost analytics, growing integration of digital claims processing platforms, expansion of specialty pharmacy management services, enhanced focus on cost containment strategies.Global Pharmacy Benefit Management Market Segmentation
1) By Services: Mail-Delivery, Specialty Pharmacy, Preferred Network Pharmacy 2) By Type: Commercial Health Plans, Self-Insured Employer Plans, Medicare Part D Plans, Federal Employees Health Benefits Program 3) By End User: Pharmacy Benefit Management Organization, Mail Order Pharmacies, Retail Pharmacies, Inpatient Pharmacies, Outpatient Pharmacies Subsegments: 1) By Mail-Delivery: Maintenance Medications, Acute Care Medications, Patient Education And Support Services 2) By Specialty Pharmacy: High-Cost Medications, Biologics And Biosimilars, Disease Management Services 3) By Preferred Network Pharmacy: Retail Pharmacy Networks, Contracted Pharmacy Networks, Urgent Care Pharmacy ServicesWhat Is The Driver Of The Pharmacy Benefit Management Market?
The increasing chronic diseases are expected to propel the growth of the pharmacy benefit management market going forward. Chronic diseases refer to long-term health conditions that persist for an extended period, typically lasting for three months or more. Pharmacy benefit management is used in managing chronic diseases for optimizing medication access, promoting adherence, and implementing cost-effective strategies, ensuring better health outcomes and quality of life for patients with long-term medical conditions. For instance, in September 2023, according to the World Health Organization (WHO), a Switzerland-based intergovernmental health organization, there were 41 million deaths, which is 74% of all deaths caused by noncommunicable diseases (NCDs) or chronic diseases every year globally. Among them are 17.9 million deaths from cardiovascular diseases, 9.3 million from cancer, 4.1 million from chronic respiratory diseases, and 2.0 million from diabetes. Therefore, increasing chronic disease is driving the growth of the pharmacy benefit management industry.Key Players In The Global Pharmacy Benefit Management Market
Major companies operating in the pharmacy benefit management market are CVS Health Corporation, Cigna Corporation, Centene Corporation, Anthem Inc., OptumRx Inc., Humana Pharmacy Solutions Inc., Magellan Health Inc., Prime Therapeutics LLC, MaxorPlus Ltd., RxAdvance Corp, MedImpact Healthcare Systems Inc., PerformRx LLC., Navitus Health Solutions LLC, WellDyneRx Inc., Healthesystems LLC., Catalyst Rx Inc., Argus Health Systems Inc., Innoviant Pharmacy Inc., Pharmaceutical Strategies Group, ProCare Rx Inc., FutureScripts LLC., National CooperativeRx, ScriptCare Ltd., US Script Inc., LDI Integrated Pharmacy Services LLC, RxPreferred Benefits, SinfoníaRx Inc.Global Pharmacy Benefit Management Market Trends and Insights
Major companies in the pharmacy benefit management market are focusing on developing innovative products such as medication therapy management, which allows for comprehensive review and optimization of a patient’s medication regimen and resolution of drug-related problems through advanced technology. Medication therapy management refers to a clinical service provided by pharmacists aimed at optimizing a patient’s medication use and improving health outcomes. For instance, in May 2025, America's TPA LLC, a US-based independent health innovator specializing in pharmacy management solutions, launched EZrx, a next-generation pharmacy solution leveraging six cost-reduction strategies, which include therapeutic substitution and prior authorization. Additionally, it also offers advanced analytics and member engagement tools to further optimize pharmacy benefit management and improve clinical outcomes.What Are Latest Mergers And Acquisitions In The Pharmacy Benefit Management Market?
In March 2025, Northwind Pharmaceuticals, a US-based pharmaceutical company focused on prescription drug solutions, partnered with Healthee to offer employers tools for cost control through enhanced transparency and benefit navigation solutions within pharmacy benefit management. Through this collaboration, Northwind aims to help employers optimize prescription drug spending and improve employee access to medications by leveraging Healthee’s advanced digital platform, which simplifies benefit navigation and provides actionable insights into drug costs. Healthee is a US-based company specializing in digital health solutions that enhance transparency and engagement in pharmacy benefits management.Regional Outlook
North America was the largest region in the pharmacy benefit management market in 2025. Asia-Pacific is expected to be the fastest-growing region in the forecast period. The regions covered in this market report are Asia-Pacific, South East Asia, Western Europe, Eastern Europe, North America, South America, Middle East, Africa. The countries covered in this market report are Australia, Brazil, China, France, Germany, India, Indonesia, Japan, Taiwan, Russia, South Korea, UK, USA, Canada, Italy, Spain.What Defines the Pharmacy Benefit Management Market?
The pharmacy benefit management market includes revenues earned by entities by providing case management, disease management, and drug utilization services. The market value includes the value of related goods sold by the service provider or included within the service offering. Only goods and services traded between entities or sold to end consumers are included.How is Market Value Defined and Measured?
The market value is defined as the revenues that enterprises gain from the sale of goods and/or services within the specified market and geography through sales, grants, or donations in terms of the currency (in USD unless otherwise specified). The revenues for a specified geography are consumption values that are revenues generated by organizations in the specified geography within the market, irrespective of where they are produced. It does not include revenues from resales along the supply chain, either further along the supply chain or as part of other products.What Key Data and Analysis Are Included in the Pharmacy Benefit Management Market Report 2026?
The pharmacy benefit management market research report is one of a series of new reports from The Business Research Company that provides market statistics, including industry global market size, regional shares, competitors with the market share, detailed market segments, market trends and opportunities, and any further data you may need to thrive in the pharmacy benefit management industry. The market research report delivers a complete perspective of everything you need, with an in-depth analysis of the current and future state of the industry.Pharmacy Benefit Management Market Report Forecast Analysis
| Report Attribute | Details |
|---|---|
| Market Size Value In 2026 | $755.09 billion |
| Revenue Forecast In 2035 | $1033.9 billion |
| Growth Rate | CAGR of 8.5% from 2026 to 2035 |
| Base Year For Estimation | 2025 |
| Actual Estimates/Historical Data | 2020-2025 |
| Forecast Period | 2026 - 2030 - 2035 |
| Market Representation | Revenue in USD Billion and CAGR from 2026 to 2035 |
| Segments Covered | Services, Type, End User |
| Regional Scope | Asia-Pacific, Western Europe, Eastern Europe, North America, South America, Middle East, Africa |
| Country Scope | The countries covered in the report are Australia, Brazil, China, France, Germany, India, ... |
| Key Companies Profiled | CVS Health Corporation, Cigna Corporation, Centene Corporation, Anthem Inc., OptumRx Inc., Humana Pharmacy Solutions Inc., Magellan Health Inc., Prime Therapeutics LLC, MaxorPlus Ltd., RxAdvance Corp, MedImpact Healthcare Systems Inc., PerformRx LLC., Navitus Health Solutions LLC, WellDyneRx Inc., Healthesystems LLC., Catalyst Rx Inc., Argus Health Systems Inc., Innoviant Pharmacy Inc., Pharmaceutical Strategies Group, ProCare Rx Inc., FutureScripts LLC., National CooperativeRx, ScriptCare Ltd., US Script Inc., LDI Integrated Pharmacy Services LLC, RxPreferred Benefits, SinfoníaRx Inc. |
| Customization Scope | Request for Customization |
| Pricing And Purchase Options | Explore Purchase Options |
