
Healthcare Fraud Detection Market Report 2026
Global Outlook – By Type (Descriptive Analytics, Predictive Analytics, Prescriptive Analytics), By Model (On-Premise Delivery, On-Demand Delivery), By Component (Services, Software ), By Application (Insurance Claims Review, Payment Integrity ), By End User (Healthcare Payers, Government Agencies, Other End-Users) - Market Size, Trends, And Global Forecast 2026-2035
Healthcare Fraud Detection Market Overview
• Healthcare Fraud Detection market size has reached to $4.66 billion in 2025 • Expected to grow to $17.83 billion in 2030 at a compound annual growth rate (CAGR) of 30.8% • Growth Driver: Surging Healthcare Fraud Incidents Fuel Growth In Healthcare Fraud Detection Market • Market Trend: Product Innovations Transforming The Healthcare Fraud Detection Market • North America was the largest region in 2025.What Is Covered Under Healthcare Fraud Detection Market?
Healthcare fraud detection refers to a group of actions performed to stop someone from obtaining patient data or property under false pretenses and involves account auditing and detective investigation. It is used to promote transparency and accountability, risk assessment by identifying data usage, detection, prevention, and management of suspicious fraud, waste, and abuse, and reduce leakage of sensitive information such as patient medical records and other credentials. The main type of healthcare fraud detection includes descriptive analytics, predictive analytics and prescriptive analytics. Descriptive analytics are used to help with predictive and prescriptive analytics to manage medical imaging scans, clinical and outcomes data. Descriptive analytics refers to the method of finding patterns and relationships by combining historical and present data to identify suspicious activities. The models include on-premises delivery and on-demand delivery, which uses components such as services and software. The application includes insurance claims review and payment integrity and are used by healthcare payers, government agencies and others.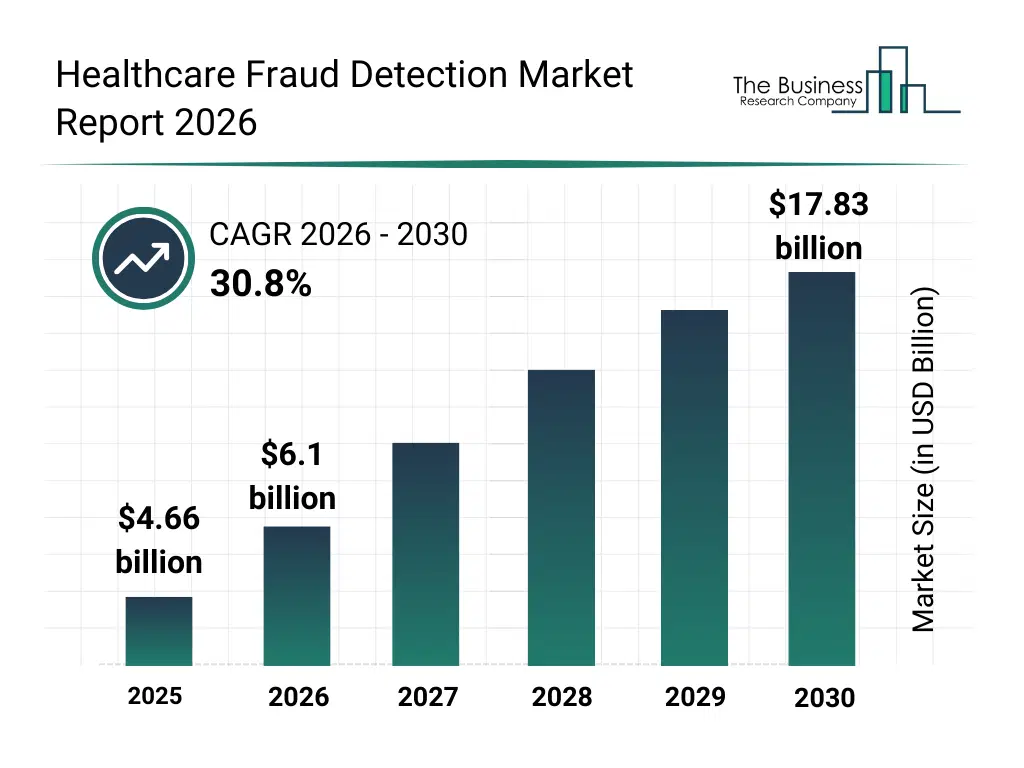
What Is The Healthcare Fraud Detection Market Size and Share 2026?
The healthcare fraud detection market size has grown exponentially in recent years. It will grow from $4.66 billion in 2025 to $6.1 billion in 2026 at a compound annual growth rate (CAGR) of 31.0%. The growth in the historic period can be attributed to increasing healthcare claims volumes, rising incidents of billing fraud and abuse, adoption of data analytics in healthcare finance, growing regulatory oversight, digitization of healthcare payment systems.What Is The Healthcare Fraud Detection Market Growth Forecast?
The healthcare fraud detection market size is expected to see exponential growth in the next few years. It will grow to $17.83 billion in 2030 at a compound annual growth rate (CAGR) of 30.8%. The growth in the forecast period can be attributed to increasing investments in advanced analytics solutions, rising demand for automated fraud prevention tools, expansion of cloud-based healthcare platforms, growing integration of machine learning in claims processing, increased focus on cost containment. Major trends in the forecast period include increasing adoption of AI-based fraud detection platforms, rising use of predictive analytics for claims review, growing deployment of real-time payment integrity solutions, expansion of cloud-based fraud detection systems, enhanced focus on data transparency and compliance.Global Healthcare Fraud Detection Market Segmentation
1) By Type: Descriptive Analytics, Predictive Analytics, Prescriptive Analytics 2) By Model: On-Premise Delivery, On-Demand Delivery 3) By Component: Services, Software 4) By Application: Insurance Claims Review, Payment Integrity 5) By End User: Healthcare Payers, Government Agencies, Other End-Users Subsegments: 1) By Descriptive Analytics: Data Mining, Reporting Tools, Historical Data Analysis 2) By Predictive Analytics: Risk Scoring Models, Machine Learning Algorithms, Trend Analysis 3) By Prescriptive Analytics: Decision Support Systems, Optimization Algorithms, Scenario Analysis And SimulationsWhat Is The Driver Of The Healthcare Fraud Detection Market?
The rise in fraudulent events in the healthcare industry is expected to propel the healthcare fraud detection market going forward. Fraudulent events in healthcare refer to the deliberate misrepresentation of patient data and insurance information in order to obtain an unfair or illegal gain or to deprive a user of a legal right. For instance, in June 2024, according to the Department of Justice, a US-based federal executive department, in 2024, Department of Justice announced a national health care fraud takedown charging 193 defendants, including 76 medical professionals, alleging about US$ 2.75 billion in intended losses and US$ 1.6 billion in actual losses. Therefore, the rise in fraudulent events in the healthcare industry is expected to drive the growth of the healthcare fraud detection industry.Key Players In The Global Healthcare Fraud Detection Market
Major companies operating in the healthcare fraud detection market are International Business Machines Corporation, Cotiviti Inc., Fair Isaac Corporation, SAS Institute Inc., RELX Group PLC, LexisNexis Risk Solutions Group, EXL Service Holdings Inc., Qlarant Inc., Change Healthcare LLC, Codoxo Inc., Pondera Solutions Inc., HMS Holdings Corp., FraudLens Inc., FraudScope Inc., Healthcare Fraud Shield LLC, MultiPlan Corporation, CGI Inc., DXC Technology Company, Conduent Incorporated, HCL Technologies Limited, Wipro Limited, H2O.ai Inc., McKesson CorporationGlobal Healthcare Fraud Detection Market Trends and Insights
Major companies operating in the healthcare fraud detection market are focusing on developing innovative solutions, such as advanced insurance fraud detection platforms, to improve real-time claim monitoring, strengthen data verification, and reduce fraudulent activity across healthcare and insurance systems. Insurance fraud detection platforms refer to integrated technology suites that utilize advanced analytics, continuous monitoring, and automated data validation to identify suspicious behavior, flag high-risk claims, and support investigators with actionable insights. For instance, in June 2023, Verisk Analytics Inc., a US-based analytics company, in collaboration with Kyndryl Holdings, Inc., launched an advanced technology suite designed to prevent insurance fraud in Israel’s compulsory insurance market. Leveraging Kyndryl’s high-performance computing capabilities and Verisk’s domain expertise, the enhanced anti-fraud engine enables real-time monitoring of auto claims for bodily injury. Supported by 24/7 managed services and sophisticated analytics, the system authenticates applicant information, cross-checks records with government and external databases, and streamlines data investigation for claim adjusters. This collaboration aims to improve claims integrity, detect fraud more effectively, and address growing consumer expectations within an increasingly digitized insurance landscape, reinforcing technological progress in the healthcare fraud detection market.What Are Latest Mergers And Acquisitions In The Healthcare Fraud Detection Market?
In July 2025, Prime Health Services, a US-based provider of healthcare payer services, clinical data management, and claims review solutions, partnered with 4L Data Intelligence to enhance its fraud, waste, and abuse (FWA) detection capabilities by leveraging advanced AI-driven risk scoring and real-time behavioral analytics. 4L Data Intelligence is a US-based provider of AI-powered healthcare analytics and risk detection solutions that help payers identify and mitigate fraudulent or abusive claims.Regional Outlook
North America was the largest region in the healthcare fraud detection market in 2025. The regions covered in this market report are Asia-Pacific, South East Asia, Western Europe, Eastern Europe, North America, South America, Middle East, Africa. The countries covered in this market report are Australia, Brazil, China, France, Germany, India, Indonesia, Japan, Taiwan, Russia, South Korea, UK, USA, Canada, Italy, Spain.What Defines the Healthcare Fraud Detection Market?
The health fraud detection market includes revenues earned by entities by tracking secondary data, providing technology specialist. The market value includes the value of related goods sold by the service provider or included within the service offering. Only goods and services traded between entities or sold to end consumers are included.How is Market Value Defined and Measured?
The market value is defined as the revenues that enterprises gain from the sale of goods and/or services within the specified market and geography through sales, grants, or donations in terms of the currency (in USD unless otherwise specified). The revenues for a specified geography are consumption values that are revenues generated by organizations in the specified geography within the market, irrespective of where they are produced. It does not include revenues from resales along the supply chain, either further along the supply chain or as part of other products.What Key Data and Analysis Are Included in the Healthcare Fraud Detection Market Report 2026?
The healthcare fraud detection market research report is one of a series of new reports from The Business Research Company that provides market statistics, including industry global market size, regional shares, competitors with the market share, detailed market segments, market trends and opportunities, and any further data you may need to thrive in the healthcare fraud detection industry. The market research report delivers a complete perspective of everything you need, with an in-depth analysis of the current and future state of the industry.Healthcare Fraud Detection Market Report Forecast Analysis
| Report Attribute | Details |
|---|---|
| Market Size Value In 2026 | $6.1 billion |
| Revenue Forecast In 2035 | $17.83 billion |
| Growth Rate | CAGR of 31.0% from 2026 to 2035 |
| Base Year For Estimation | 2025 |
| Actual Estimates/Historical Data | 2020-2025 |
| Forecast Period | 2026 - 2030 - 2035 |
| Market Representation | Revenue in USD Billion and CAGR from 2026 to 2035 |
| Segments Covered | Type, Model, Component, Application, End User |
| Regional Scope | Asia-Pacific, Western Europe, Eastern Europe, North America, South America, Middle East, Africa |
| Country Scope | The countries covered in the report are Australia, Brazil, China, France, Germany, India, ... |
| Key Companies Profiled | International Business Machines Corporation, Cotiviti Inc., Fair Isaac Corporation, SAS Institute Inc., RELX Group PLC, LexisNexis Risk Solutions Group, EXL Service Holdings Inc., Qlarant Inc., Change Healthcare LLC, Codoxo Inc., Pondera Solutions Inc., HMS Holdings Corp., FraudLens Inc., FraudScope Inc., Healthcare Fraud Shield LLC, MultiPlan Corporation, CGI Inc., DXC Technology Company, Conduent Incorporated, HCL Technologies Limited, Wipro Limited, H2O.ai Inc., McKesson Corporation |
| Customization Scope | Request for Customization |
| Pricing And Purchase Options | Explore Purchase Options |
